Entry to care impacts individuals with epilepsy worldwide. Bringing care nearer to house can assist—however what about bringing care inside the house?
The first remedy hole consists of people that have epilepsy and are usually not receiving remedy. There’s one other group of individuals: those that are identified however cease taking their medicine, making a secondary epilepsy remedy hole. There are various causes for this remedy hole, together with adversarial results of anti-seizure drugs (ASMs), value of medicines, entry to drugs, and a lack of knowledge amongst individuals with epilepsy about how the drugs work and the significance of taking them as prescribed.
Bringing care nearer to individuals’s houses can cut back the secondary remedy hole. In international locations with low numbers of neurologists, the World Well being Group encourages the supply of epilepsy care by major well being care suppliers. For individuals in rural or distant areas, this closes the gap between house and clinic, growing the probabilities of remedy adherence.
Residence supply of epilepsy care is one other alternative to cut back the secondary remedy hole. Care is given by educated staff regularly, who additionally present drugs. This mannequin of care ensures medicine supply to the particular person with epilepsy and offers alternatives for adherence monitoring and counseling on self-management. These features might enhance adherence and result in higher seizure management.
To guage this concept, a latest randomized trial in contrast home-based epilepsy care to clinic-based care over a two-year interval in Ludhiana, India. Twenty-four geographic clusters, every composed of 10 individuals with epilepsy, had been randomized to both home-based care or clinic-based care.
Researchers accomplished a door-to-door survey in a number of areas of town, figuring out individuals with epilepsy. These recognized had been invited for a neurological analysis, together with EEG and MRI, to substantiate an epilepsy analysis. They had been then invited to participate within the examine, which is now revealed within the journal Epilepsia Open.
Clinic-based care
Folks attended clinic on the authorities district hospital as soon as a month, the place they had been seen by a neurologist. They acquired routine recommendation and data and had been supplied with ASMs without charge.
“There may be really no neurologist within the district hospital in Ludhiana,” stated Gagandeep Singh, the examine’s principal investigator, a neurologist and professor in north India. “In reality, in most cities in India, the district hospital doesn’t have a neurologist. However our Well being Minister stated that for this examine, we might have a neurologist go to the hospital as soon as per week to see sufferers with epilepsy.”
Residence-based care
Folks acquired month-to-month visits from neighborhood well being staff or nurses, who offered ASMs without charge. The well being staff additionally recommended individuals about stigma administration, epilepsy self-management, first help, and the significance of medicine adherence.
The neighborhood well being staff in Ludhiana are ASHA staff, the spine of India’s neighborhood well being program. They focus totally on reproductive well being and immunizations; examine researchers educated them to dispense ASMs to individuals with epilepsy and to offer steering round adherence and self-management.
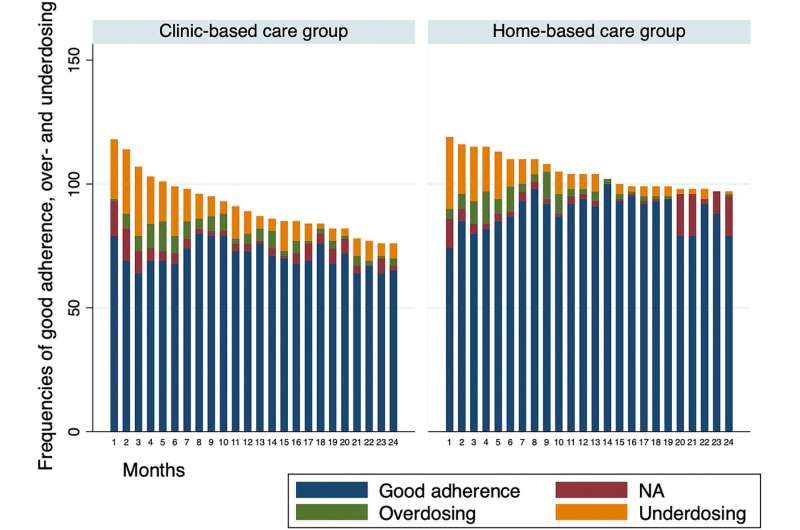
Residence-based care related to higher adherence and fewer seizures
After two years, “There have been a lot much less individuals within the house care arm that dropped out,” stated Dr. Singh. “Their adherence was considerably higher, and their seizure management was additionally considerably higher.”
By the top of the trial, 37% of individuals in clinic-based care had left the examine, in contrast with 19% in home-based care. Causes for dropping out had been diverse.
Residence care recipients had been 1.8 occasions as more likely to be adherent to their ASMs, in contrast with individuals in clinic-based care.
“Individuals who have to come back and gather their medicines, even when they’re freed from value, they may nonetheless not come,” stated Dr. Singh. “Coming to the clinic may cost somewhat bit [for transportation], however extra typically what it does is individuals lose in the future of wages. And that is quite a bit for them.”
Nonetheless, when drugs are offered at house, “adherence is best, compliance is best—it is a lot easier for them to take the medicines,” he stated.
Folks within the home-care arm might nonetheless go to the clinic on the recommendation of a well being care supplier, and people within the clinic-care arm might make visits outdoors the common schedule. Hospitalization charges had been about the identical in each teams.
Studying from hypertension analysis
India’s public well being system was created to handle infectious illness somewhat than continual illness, stated Dr. Meenakshi Sharma, creator of the examine and a scientist and program officer with the Indian Council of Medical Analysis. She stated that research on treating hypertension even have highlighted the effectiveness of extra localized remedy. Research discovered that management charges for extra localized care averaged 60% to 65%, whereas management charges at district hospitals had been round 35%.
“We have now to offer methods by which medication will be offered nearer to the house of the affected person,” she stated. For hypertension management initiatives, researchers calculated the quantities of medicine that had been wanted, and caught to 2 or three forms of anti-hypertensives. “The procurement of the medication turned simpler, and we might provide major well being facilities and well being and wellness facilities,” she stated. Sufferers additionally got 30-day provides somewhat than 7-day provides, to cut back the necessity for visits.
For epilepsy care, “We have now to guarantee that the medication can be found at our major well being care heart stage,” she stated. A system of care, tailored from hypertension initiatives, would possibly look one thing like this:
- Folks suspected of getting epilepsy are transferred to the district hospital stage for analysis and remedy initiation.
- As soon as steady, they’re shifted again to the first well being care stage, the place they’re managed and drugs is disbursed.
Adherence was measured with tablet counts; individuals whose counts had been off by greater than two drugs had been thought-about non-adherent.”
That is what has been performed in earlier [epilepsy] research,” stated Dr. Singh. “In situations like hypertension, the bar for adherence is one thing like 80%. However epilepsy is a situation that if individuals miss even a single tablet, they’re in danger. That’s the reason we used this stringent criterion.”
Bettering care by training
“Remedy actually wants to come back nearer to house,” stated Dr. Singh. “And first care training with regard to epilepsy is extraordinarily vital.” He famous that to fulfill the objectives of the Intersectoral World Motion Plan (IGAP), many low-resource areas might want to be sure that major care personnel are educated about epilepsy.
Educating individuals with epilepsy about their situation is also essential in initiatives to shrink the remedy hole, stated Dr. Singh. “Most individuals in resource-limited communities consider medication or well being care as one thing that’s mainly meant for acute situations, or situations that are extraordinarily critical,” he stated. “Within the case of somebody with epilepsy, the particular person has acute seizures or standing epilepticus, will go to the hospital, get remedy, come again house, take remedy for a while after which cease taking remedy. Then after a number of weeks or months or years, once more they’ve seizures and once more they’ve issues.”
In Dr. Singh’s examine, greater than 90% of individuals had lower than a high-school training. “I believe well being literacy about epilepsy remedy has quite a bit to do with primary ranges of training,” he stated.
Dr. Sharma agreed. “As soon as now we have arrange a facility as a well being heart, we face the problem that the affected person both would not come to the hospital to take the required remedy or get the analysis, or he would not adhere to the remedy.”
Folks with epilepsy additionally have a tendency to go to conventional healers as properly, she stated. “We have to have social scientists with us, understanding what is going on locally and methods to change health-seeking behaviors. That is a giant problem, not just for epilepsy however for all non-communicable illnesses.”
How can these outcomes apply to different areas of the world?
Even inside India, there are totally different geographical and sociocultural environments, stated Dr. Singh. “One has to search out out one of the best ways of addressing the remedy hole, reducing burden, reducing morbidity and mortality. We have to take a look at it from a wider angle, which most likely consists of extra specialist involvement, major care training, neighborhood consciousness—there are such a lot of issues that should be constructed up right into a complete mannequin of take care of epilepsy.”
Dr. Sharma agreed. “One mannequin will not be going to slot in each place. And for areas the place now we have specialists, now we have to assume in a hub-and-spoke type of mannequin. For areas the place there isn’t any close by medical school or district hospital, now we have to take a look at totally different sorts of challenges and construct a mannequin accordingly.”
She stated the home-care examine has expanded understanding of how the well being care system works from the affected person’s viewpoint. Neighborhood messages—epilepsy is treatable, adherence is essential—should be initiated and repeated to ultimately enhance individuals’s understanding and willingness to enter and stay within the well being care system.
“I am very certain we will give you two or three totally different fashions that are going to cater to the regional variations in our nation,” she stated. “However that is going to be a protracted journey.”
Extra data:
Gagandeep Singh et al, A cluster‐randomized trial evaluating house‐primarily based major well being care and normal clinic take care of epilepsy in a useful resource‐restricted nation, Epilepsia Open (2022). DOI: 10.1002/epi4.12659
Offered by
Worldwide League Towards Epilepsy
Quotation:
Bringing epilepsy care nearer to house might enhance outcomes (2023, June 19)
retrieved 19 June 2023
from https://medicalxpress.com/information/2023-06-epilepsy-closer-home-outcomes.html
This doc is topic to copyright. Other than any honest dealing for the aim of personal examine or analysis, no
half could also be reproduced with out the written permission. The content material is offered for data functions solely.




